What is Leukemia
Normal Blood
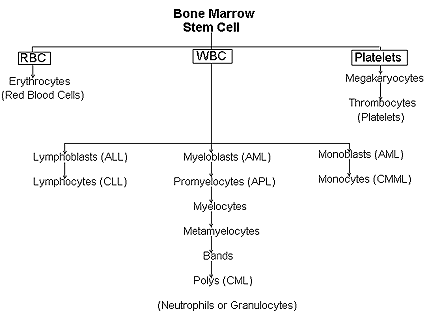
To better understand what happens to the blood when you have leukemia, it is helpful to know about normal blood and bone marrow. There are only three major types of blood cells: red blood cells (RBCs), white blood cells (WBCs), and platelets. These cells are produced in the bone marrow and circulate through the blood stream in a liquid called plasma.
Red Blood Cells (RBCs), the major component of blood, carry oxygen and carbon dioxide throughout your body. The percentage of RBCs in the blood is called the hematocrit. The part of the RBC that carries oxygen is a protein called hemoglobin. All body tissues need oxygen to function properly. When the bone marrow is functioning normally, the RBC count remains stable. Anemia occurs when there are too few RBCs in the body. The leukemia itself or the chemotherapy used to treat it can cause anemia, whose symptoms include shortness of breath, weakness, and fatigue.
Some people will have symptoms of anemia when the hemoglobin value is more than 8, depending on their other medical conditions, but most people will have some symptoms when the hemoglobin is less than 8. This is why blood transfusions are frequently ordered when the hemoglobin is less than 8.
White Blood cells (WBCS) - There are several different types of white blood cells, each with their own function in protecting the body from germs. Three major types include: neutrophils, monocytes, and lymphocytes. Neutrophils are the same cells as neuts, granulocytes, polys, or PMN's (just different names). Neutrophils kill most regular bacteria. You can see them accumulate as pus with an infected wound on your skin. Monocytes kill germs such as tuberculosis. Lymphocytes are responsible for killing viruses and for overall management of the immune system. Lymphocytes recognize foreign material and increase the body's resistance to infection. WBCs play a major role in fighting infection. Infections are therefore more likely to occur when there are too few normal WBCs in the body.
Absolute Neutrophil Count (ANC) is a test used to measure the amount of WBCs you have to fight infections. You can figure out your ANC by multiplying the total number of WBCs by the percentage of neutrophils ("neuts"). The percentage of the various cells is what makes up the diff (or differential or basically what is the percentage breakdown of the different kinds of white blood cells). For example:
Let's say your WBC = 1000 = 1.0 K (K = kilo which means thousands)
And your percentage of neutrophils = 50% (you can find this number on your "diff")
Therefore your absolute neutrophil count is 50% of 1000 = 500.
Does that seem difficult? If you have ever made a purchase, we can put it another way:
Let's say you buy a TV for $1000
And you have to pay a sales tax = 50%
Then your sales tax is 50% of $1000 = $500
Even with that big sales tax rate, a purchase for only $1 would "only" cost you 50 cents in tax, so for the same percent of neuts, the higher your WBC, the higher your absolute neutrophil count.
While any of us can catch a cold or other infections, serious infections are more likely to occur when your ANC falls below 500 and very likely if your ANC is less than 100. Your WBC will generally fall within the first week after starting chemotherapy. Most people recover their WBC count anywhere between 21 to 28 days after starting chemotherapy.
Platelets are the cells that help control bleeding. When you cut yourself, the platelets collect at the site of the injury and form a plug to stop the bleeding. The risk of bleeding is always proportional to the amount of trauma sustained (don't forget to stop at all railroad crossings!), but the risk of bleeding increases substantially when the platelet count is less than 10-20,000. The risk of bleeding increases if you have taken aspirin, motrin or other anti-inflammatory drugs, but Tylenol has no effect on platelets.
Bone Marrow is the soft tissue within the bones where blood cells are produced. All blood cells begin in the bone marrow as blast or stem cells. Blast cells are very immature cells. They function as the seeds of the marrow. When the need arises, the blast cells are signaled to develop into mature RBCs, WBCs or platelets. These useful cells can no longer divide to keep the system going. Leukemic blasts look like the normal life-sustaining blasts, but when they divide, they generate blasts that cannot differentiate. They accumulate in the marrow as islands or mounds of blasts. It is the accumulation of blasts that is so abnormal in acute leukemia.
The bone marrow is composed of blood cells at different stages of maturation. As each cell fully matures, it is released from the bone marrow to circulate in the blood stream. The blood circulating outside of the bone marrow in the heart, veins, and arteries is called peripheral blood. Therefore, when you hear someone speak of the peripheral blood or cells in the periphery, they are speaking of the blood and cells outside of the bone marrow.
The specific cause of leukemia is still not known. Scientists suspect that viral, genetic, environmental, or immunologic factors may be involved.
Some viruses cause leukemia in animals; but in humans, viruses cause only one rare type of leukemia. Even if a virus is involved, leukemia is not contagious. There is no increased incidence of leukemia among people (friends, family, care givers) who have close contact with leukemia patients.
There may be a genetic predisposition to leukemia. There are rare families where people born with Chromosome damage may have genes that increase their chances of developing leukemia.
Environmental factors such as high-dose radiation and exposure to certain toxic chemicals have been directly related to leukemia, but only in extreme cases, such as atomic bomb survivors in Nagasaki and Hiroshima or industrial workers exposed to benzene. Controlled exposure to ordinary x-rays, like chest x-rays, is not believed to be dangerous.
Finally, people with immune system deficiencies appear to be at more risk for cancer because of the body's decreased ability to resist foreign cells. There is evidence that patients treated for other types of cancer with some types of chemotherapy and/or high-dose radiation therapy may develop leukemia later on.
All of these factors may account for a small number of the people with leukemia. Again, among the majority of people, the cause is not known.
Leukemia is cancer of blood-forming tissue such as bone marrow. Types of leukemia are classified by the type of cell affected and by the rate of cell growth. Leukemia may be either classified as acute or chronic.
Acute leukemia involves an overgrowth of very immature blood cells. This condition is life threatening because there are not enough mature blood cells to prevent anemia, infection, and bleeding.
Chronic leukemia involves an overgrowth of very mature blood cells. Usually, people with chronic leukemia have enough mature blood cells to prevent serious bleeding and infection.
Myelodysplastic Syndrome (MDS) is a condition in which the bone marrow does not function normally and therefore does not produce enough normal blood cells. The blood cells affected are white blood cells, red blood cells, and platelets.
Different forms of leukemia tend to be linked with certain age groups. Acute lymphoblastic leukemia is most common during childhood and in early adulthood, although it is also diagnosed in adults 30 years and older. Acute myelogenous leukemia occurs more often in adults. Chronic leukemia is more prevalent between ages 40 and 70 and is rare among young people. MDS is most often found in patients nearing their 60s and 70's. However, there are always exceptions.
Doctors identify a specific type of leukemia on the basis of chromosome number and appearance, features on the bone marrow cell surface, and the appearance of the bone marrow cells under microscope. The following is a list of the different types of leukemia. Classification numbers for the French American Britain (FAB) system are given in brackets [ ].
Myeloid
Lymphoid
Myeloid
Lymphoid

The diagnosis of leukemia is based on the results of both blood and bone marrow tests such as bone marrow aspiration and bone marrow biopsy. Before insertion of the bone marrow aspiration needle, the aspiration site is numbed with local anesthesia. During bone marrow aspiration, a sample of bone marrow cells is removed from the hip bone with a needle. Most people feel pressure as the needle is inserted and a few seconds of pain when the bone marrow fluid is withdrawn. With a bone marrow biopsy a small piece of bone is removed. A biopsy may be slightly more painful, but only during the time that the procedure is being done.